When Can You Lift Weights After Hernia Surgery
Abstract
Groundwork
There are no valid recommendations or reliable guidelines bachelor to guide patients how long they should refrain from lifting weights or returning to heavy physical labor subsequently intestinal or hernia surgery. Recent studies plant that surgeons' recommendations non to be evidence-based and might exist too restrictive because data on fascial healing and incisional hernia development. It is likely that this impairs the patient'southward quality of life and leads to remarkable socio-economical costs. Hence, nosotros conducted this survey to gather international expert's opinions on this topic.
Materials and methods
At the 41st Annual International Congress of the EHS, attending international experts were asked to complete a questionnaire concerning recommendations on given proposals for postoperative refrain from heavy work or lifting after abdominal surgery and too after hernia repairs.
Results
In full, 127 experts took part in the survey. 83.9% were consultants with a mean experience since specialization of more than eleven years. Two weeks of no heavy concrete strain subsequently laparoscopic surgery were considered sufficient by more than than 50% of the participants. For laparotomy, more than 50% rated four weeks appropriate. For mesh-augmented sublay and IPOM repair of ventral or incisional hernias, more than than l% rated iv weeks of rest appropriate. For complex hernia repair, 37% rated 4 weeks reasonable. Two weeks later, groin hernia surgery was considered sufficient by more than than l% of the participants.
Conclusion
Following groin hernia repair (Lichtenstein/endoscopic technique) and laparoscopic operation, the majority agreed on the proposal of ii weeks refraining from physical strain. Four weeks of no concrete strain were considered appropriate past a majority later laparotomy and open up incisional hernia repair. However, the results showed substantial variation in the ratings, which indicates uncertainty even in this selected accomplice of hernia surgery experts and emphasizes the demand for further scientific evaluation. This is specially remarkable, considering a lack of evidence that early on postoperative strain leads to higher incisional hernia rates.
Trial registration
Number DRKS00023887.
Introduction
Surgical procedures underwent a technical development in the recent three decades. Due to the further development of minimally invasive techniques and implementation of enhanced recovery subsequently surgery protocols (ERAS), length of hospital stay decreased and early mobilization became an essential element in the postoperative course [1].
Nevertheless, the occurrence or recurrence of incisional hernias subsequently abdominal or hernia surgery is a common complication, equally they are reported in 12.viii% within the first two years of abdominal surgery. [2] A negative impact of early on postoperative concrete strain, that might lead to fascial vehement or trauma and, hence, to loftier incisional hernia rates is widely suspected [3].
That might exist reflected in the postoperative recommendations given to patients. Of import elements of postoperative management are those recommendations of convalescence, especially regarding physical activity and render to piece of work. The advice given to patients by their surgeons directly affects the patients' behavior, their participation in daily and social life and, of grade, the elapsing of ill go out and return to work. How long patients should refrain from lifting weights or returning to regular concrete activity after abdominal or hernia surgery is debated and information from hernia inquiry emphasize a major impact of collagen metabolism in the pathogenesis of incisional or main ventral hernias [iv, 5].
Study data from Germany prove a considerable variance of recommendations given to patients [5]. Moreover, such proposals are non prove-based and might be too restrictive, considering the available data on fascial healing and incisional hernia development.
For inguinal hernia repair, it could be shown that there is an extensive database, and at that place is no show which justifies restrictive recommendations [six, vii]. Also, even no restriction or simply a few days is not associated with higher rates of complications or recurrences. Hence, the International Guidelines for Groin Hernia Management emphasized that patients should be encouraged to return to their normal activities as shortly as possible (upgrade to strong recommendation). [8]
Such a conclusive database does not exist for intestinal or incisional/ventral hernia surgery and thus, guidance of patients in the postoperative period cannot be validated by scientific results, nonetheless. To further evaluate this unanswered question, we conducted this survey to get together international expert'due south opinions on this topic. The results accept to be interpreted with regard of beingness low level of prove: level D according to Class guidelines [ix] as the Class guidelines might be of more than widespread use compared to Hadorn or Oxford classification. Practiced console statements might be biased, thus the given recommendations are not binding.
Materials and methods
At the 41st Annual International Congress of the EHS 11—14 September 2022 in Hamburg, attending experts were asked to complete a questionnaire. We included only active active surgeons with a cocky-reported special involvement (i.e., active research) and/or superior experience in that field. The only personal information collected was the profession (resident/consultant) and the duration since graduation/specialization. We asked for recommendations on given proposals for postoperative refrain from heavy work or lifting.
4 weeks of refrain from heavy work and activeness were given interval as proposal for abdominal surgery with vertical midline or transverse laparotomy and two weeks for laparoscopic surgery. 4 weeks were the given interval every bit a proposal for incisional hernia repair (sublay, IPOM (intraperitoneal onlay mesh), onlay or complex repair). Circuitous repair was considered techniques such equally transversus abdominis release or component separation techniques. Two weeks were proposed for groin hernia repair (Lichtenstein or endoscopic repair with TEP/TAPP). The proposals were to be qualified too curt, too long, or appropriate. If non suitable, the experts were asked to give their recommendations (Fig. 1). This study was intended to add together some testify in terms of evaluating the acceptance of the given proposals. Those were based on the conclusions fatigued from a German hospital survey and literature review on postoperative refrain from heavy piece of work and activity [v].

Delineation of the questionnaire used for the survey
The participation of experts was voluntary, and no benefits were offered. Also, no personal data were recorded in addition to the answers given in the questionnaire.
After the end of the survey, the data were recorded and descriptively analyzed with Excel (vs. 2016, Microsoft, Redmont, Washington, United states of america) and SPSS (vs. twenty, IBM, Armonk, New York, Us). Differences betwixt the ratings were tested for significance with the Chi-squared test. The level of significance was set to p = 0.05.
Results
In full, 127 experts took office in the survey. 83.9% were consultants with a hateful experience since specialization of about 11 years. The remaining 16.1% were residents and reported nearly 4 years since graduation. The post-obit results did not differ between the subgroups of the residents and consultants; therefore, we report the groups together.
Abdominal surgery
The given proposal was four weeks for vertical midline and transverse laparotomy, which was constitute to be advisable in 56.7/52.viii%, too short in 31.v/29.9% (recommendation 6–12 weeks), and as well long in 11.8% in both cases (recommendation one–3 weeks).
2 weeks were proposed for laparoscopy, which was rated advisable in 57.5%, in only 4.seven% equally too short (recommendation 4 weeks), and 36.2% as too long (recommendation 0–1.5 weeks). These differences were statistically significant (p = 0.000; Chi-squared examination).
Almost lxx% considered an interval of up to 4 weeks sufficient after open abdominal surgery (midline and transverse incisions). The ratings were fifty-fifty more straightforward for laparoscopy, equally more than than 90% recommended 2 weeks or shorter of reduced physical activity or lifting after laparoscopic surgery (Fig. two).
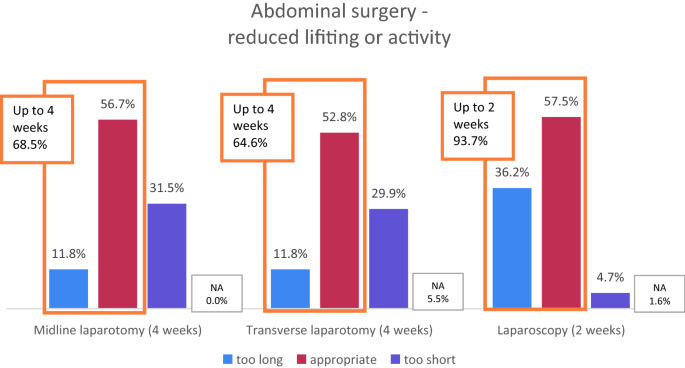
Ratings of 4 weeks for open abdominal surgery (midline or transverse laparotomy) and 2 weeks for laparoscopy. NA not answered
Groin hernia repair
For groin hernia repair, the given proposal was two weeks. That was rated appropriate in 55.9% for open repair (Lichtenstein) or 59.8% for endoscopic repair (TEP/TAPP). It was ranked likewise short in 31.5/11.0% (Lichtenstein/endoscopic) and too long in 11.viii/28.3% (Lichtenstein/endoscopic TEP-TAPP). These differences were statistically pregnant (p = 0.000; Chi-squared test). The proposed intervals were either 0–one weeks for those who rated 2 weeks also long and three–16 weeks for those who considered 2 weeks also brusk.
It was found that the majority of 58–68% considered up to 2 weeks of reduced concrete activeness or heavy lifting after a groin hernia repair to be sufficient (Fig. 3). A remarkable proportion of almost i 3rd (28%) rated 2 weeks even too long after endoscopic groin hernia repair (Fig. 3).
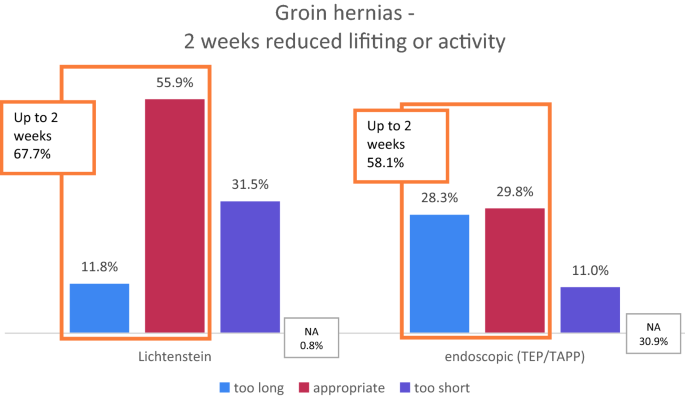
Ratings of 2 weeks reduced physical activity after groin hernia surgery. NA not answered
Incisional/ventral hernia repair
The given interval was four weeks for hernia repair. The results are shown in Table 1. For sublay, 55.1% rated it advisable, while it was too short for 31.5% and also long for thirteen.iv%. Those who rated too long recommended intervals of two–3 weeks, and those who rated likewise short suggested 5–12 weeks with a hateful of 7 weeks.
For IPOM, a like proportion of 52.0% rated 4 weeks advisable. The remaining rated every bit distributed likewise short or besides long. The recommended intervals were most the same as for sublay.
4 weeks were rated appropriate for onlay repair in 39.4%. A big proportion qualified information technology as too short (37.0%). Only a few rated too long (five.five%). About 18.1% did not charge per unit the proposal for onlay repair.
Most specialists asked (47.ii%) considered 4 weeks equally too short for circuitous hernia repair and suggested 5–16 weeks. 37.0% rated appropriate instead; only 7.one% plant it to be too long. The differences in the ratings between the surgical procedures were statistically meaning (p = 0.000, Chi-squared test).
Put together, 4 weeks of reduced lifting or physical labor was appropriate for the bulk after incisional or ventral hernia repair with sublay, IPOM, or onlay. Virtually a 3rd advocated longer intervals of seven weeks or longer. However, the data also showed that sixty–70% considered 4 weeks or shorter for sublay and IPOM reasonable (Fig. 4).
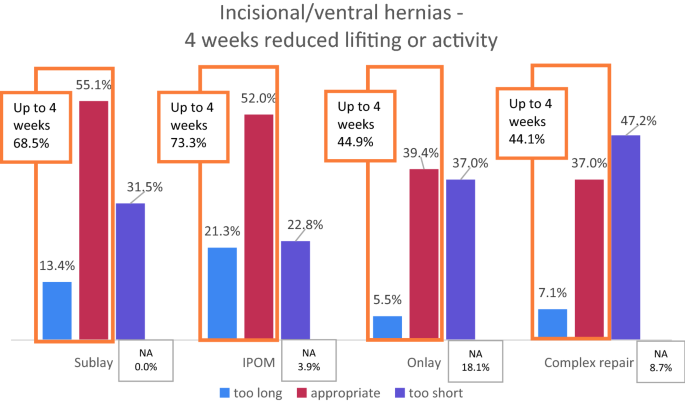
Ratings of iv weeks reduced physical activity subsequently incisional or ventral hernia surgery. IPOM intraperitoneal onlay mesh, NA not answered
Discussion
The results of this survey were based on opinions of attending surgeons of the 41st Annual Coming together of the European Hernia Society. Nosotros found pregnant variability in the ratings of the given proposals for restrictions of concrete activity. Still, our given recommendations were already quite liberal. We saw lx–70% of the participating hernia surgery experts to consider them appropriate or even besides long, namely for sublay, IPOM, both open and endoscopic inguinal hernia repair, and midline or transverse laparotomy. The proportion of participants who qualified ii weeks of reduced activeness as too long or advisable counted 94% for laparoscopy.
Possible reasons to justify restrictive recommendations for convalescence after abdominal or hernia surgery are the risk of recurrence or evolution of incisional hernias, the fright of causing mesh-related complications, or only pain. Those risks cannot be substantiated by published information and are based mainly on theoretical considerations [x, eleven]. For inguinal hernia repair, it has been shown that early and progressive strain or the immediate return to physical work is not associated with hernia recurrence. Consequently, the recommendations for the postoperative recovery to full physical activity take changed and are quite progressive nowadays [8].
Concrete strain and fascial shear stress
I central aspect is the rising intraabdominal pressure level associated with lifting. It has been shown that the increase of intraabdominal pressure is dependent on the amount of weight and the mode how it is lifted [12]. Moreover, it has been shown that fifty-fifty lifting a weight of 50 kg led to a negligible rise oof the intraabdominal pressure [thirteen]. Of grade, physical activity and lifting weights can easily be adapted in the postoperative period, simply the effect of these restrictions should be questioned and the impact of lifting weights on intraabdominal force per unit area and fascial shear stress might be overestimated. Some studies institute involuntary actions such every bit coughing, wheezing, or defecation to crusade faster and more significant increases of intraabdominal pressure, which were manner higher than that acquired by physical activity or lifting [xiv, 15].
From a biological perspective, the abdominal wall is considered to reach its full forcefulness 3–4 weeks after abdominal surgery [xvi]. Besides, fascial fibroblasts may exist activated through concrete activity, and fascia might heal faster than the skin incision in plow [17, xviii]. If the implantation of a mesh is considered, the physical properties of the operated abdominal wall are farther ameliorated. Data from inguinal hernia repair studies emphasized that the intestinal wall is stable on a physiological level immediately after mesh-augmented inguinal hernia repair [6].
A further aspect that stands against the possible negative impact of early strain is the long interval betwixt fascial trauma, i.e., abdominal or hernia surgery, and hernias' occurrence or recurrence. Information technology has been shown that the bulk of incisional hernias occur later on 1 twelvemonth or more (at least l–60%), and only under 10% developed within ane year from surgery [five, 19, 20]. Impaired collagen metabolism.
Primary ventral or inguinal hernia development is most likely acquired past impaired collagen metabolism [21, 22], which cannot be affected by postoperative resting. Other factors associated with incisional hernia development are the technique of intestinal wall closure, surgical site infections, or comorbidities like obesity or aortic aneurysms [xi]. Thus, meshes' prophylactic implantation afterward laparotomies is under investigation, equally promising results in terms of reduced incisional hernia rates accept been shown in high-risk patients [23].
Evidence for intestinal surgery
In a High german hospital surgeons survey, most of the physicians stated they gave recommendations to their patients concerning postoperative strain later abdominal surgery (93% after laparotomies, 77% afterward laparoscopies) [5]. Nonetheless, that report reveals ninety% of those recommendations were only based on individual or expert opinions rather than bachelor evidence [5].
Evidence for incisional/ventral hernia surgery
For incisional hernia surgery, Dietz et al. recommended an interval of postoperative reduced activity or lifting restrictions for iii–6 weeks in a contempo review [4]. Nevertheless, they too stated at that place is no definitive prove to give bounden recommendations. A recently published written report found considerable variation in published recommendations on the postoperative strain, a lack of evidence for the guidance given, and, in line with the survey results in this report, substantial variation, and incertitude of the surgeons, who are supposed to guide their patients [5]. Interesting insights might exist expected by a randomized controlled trial that is currently recruiting patients to evaluate the bear on of early physical training of the intestinal wall muscles after intestinal surgery on hurting, wound healing, and incisional hernia development (https://www.clinicaltrials.gov/ct2/show/NCT03808584#contacts, lastly accessed on Nov 3, 2020).
Evidence for groin hernia surgery
The Hernia Surge Written report Group published guidelines for inguinal hernia repair. Based on the available evidence, they concluded that there is no demand for postoperative activity restrictions after unproblematic inguinal hernia repair [8]. Moreover, there is no evidence that this would lead to higher inguinal hernia recurrence rates [8]. Consequently, the authors ended that piece of work or leisure activities could safely be resumed after three–5 days, both later on open up or endoscopic inguinal hernia repair [8].
Of course, inguinal hernia repair's pathophysiological weather cannot readily be adapted in abdominal surgery or open up hernia repair. Based on this study's findings and the review of the current literature, an early postoperative return to daily life activities in elementary cases might be reasonable and should be farther evaluated in prospective design. In our experience, the limit is the individual occurrence of pain (individual full strain). In special weather, complicated cases or based on an individual therapeutic decision by the surgeon, a substantially longer durations—especially in complex and big hernia repairs—might be recommended.
The resume of full physical strain, sports, and difficult work is considered possible after ii weeks for laparoscopy and inguinal hernia and subsequently iv weeks for laparotomy and open ventral/incisional hernia repair. In the author's stance, recommendations should non exceed 4 weeks afterward uncomplicated surgery to decrease the chance of unnecessarily long immobilization or sick leave.
Limitations and controversies
The results are based on expert opinions, which does not accept into account the private misreckoning factors that are relevant in enhancing or impeding the general wound and tissue repair and healing after whatsoever hernia repair (east.g., age, comorbidities, lifestyle and profession, patient's compliance and insight). That bears an inherent risk of substantial bias. Therefore, the aforementioned statement is simply recommended for uncomplicated cases, or after a complication (e.g., a surgical site infection) has already resolved. Also, whether early postoperative return to full activity and strain increases the hazard for other complications than hernia evolution or recurrence (i.e., seroma germination and inflammatory reaction) could be debated and might limit the return to full activity and strain. That needs to be addressed in prospective studies and has to exist discussed in that context.
Moreover, it should be noted that there is a lack of well-designed studies, especially for abdominal surgery, ventral or incisional hernia repair and there is a substantial risk for bias as not every patient is seen for follow-up by the initial surgeon. Nevertheless, we assume usual follow-up rates in hernia surgery to exist quite high. In our ain experience (Germany), postoperative follow-up rates of at least 70% are necessary to meet quality assurance programs' requirements in hernia surgery require average follow-up rates of at to the lowest degree 70%. Nosotros assume there are similar weather condition in other countries (i.e., western Europe/United states). Theoretically, that bears the risk of underestimation of complications, incisional or recurrent hernia development, as the surgeons just are non enlightened of the true rate of complications. To our knowledge, at that place is no evidence that patients, who suffer from complications or hernia recurrences, are more prone to be lost to follow-up to their surgeon, that aspect might be relevant for interpreting our results.
The results of this written report are based on expert opinions which is simply level of evidence D according to Form [9]. Every bit evidence-based, validated guidance is needed in clinical routine, recommendations, and convalescence regimes after intestinal and hernia surgery need to exist prospectively evaluated.
To conclude, following groin hernia repair (Lichtenstein/endoscopic technique) and laparoscopic functioning, the majority agreed on the proposal of 2 weeks refraining from physical strain. Iv weeks of no concrete strain were considered appropriate by a majority after laparotomy and open incisional hernia repair. Still, the results showed substantial variation in the ratings, which indicates doubt even in this selected accomplice of hernia surgery experts and emphasizes the need for farther scientific evaluation. This is particularly remarkable, because a lack of evidence that early postoperative strain leads to college incisional hernia rates.
Availability of information and materials
Data tables and analysis results tin can be requested via email from the respective author.
References
-
Visioni A, Shah R, Gabriel E et al (2018) Enhanced recovery after surgery for noncolorectal surgery?: A systematic review and meta-assay of major abdominal surgery. Ann Surg 267(1):57–65. https://doi.org/10.1097/SLA.0000000000002267
-
Bosanquet DC, Ansell J, Abdelrahman T et al (2015) Systematic review and meta-regression of factors affecting midline incisional hernia rates: analysis of 14,618 patients. PLoS ONE ten(9):e0138745. https://doi.org/10.1371/journal.pone.0138745
-
Paasch C, Lorenz E, Anders S et al (2019) Patient reported result post-obit incisional hernia repair: a survey on 163 patients at two maximum intendance hospitals. Ann Med Surg (Lond) 44:5–12. https://doi.org/ten.1016/j.amsu.2019.06.005
-
Dietz UA, Menzel S, Lock J et al (2018) The Treatment of Incisional Hernia. Dtsch Arztebl Int 115(3):31–37. https://doi.org/x.3238/arztebl.2018.0031
-
Güsgen C, Willms A, Schaaf South et al (2020) Lack of standardized communication on physical strain following abdominal surgery. Deutsches Aerzteblatt Online. https://doi.org/10.3238/arztebl.2020.0737
-
Buhck H, Untied Thou, Bechstein WO (2012) Evidence-based cess of the period of concrete inactivity required later inguinal herniotomy. Langenbecks Curvation Surg 397(8):1209–1214. https://doi.org/x.1007/s00423-012-1008-seven
-
Tolver MA, Rosenberg J, Bisgaard T (2016) Convalescence after laparoscopic inguinal hernia repair: a qualitative systematic review. Surg Endosc thirty(12):5165–5172. https://doi.org/10.1007/s00464-016-4863-iv
-
Simons MP, Smietanski M, Bonjer HJ et al (2018) International guidelines for groin hernia management. Hernia 22(1):i–165. https://doi.org/x.1007/s10029-017-1668-10
-
Guyatt GH, Oxman AD, Vist GE et al (2008) Grade: an emerging consensus on rating quality of bear witness and force of recommendations. BMJ 336:924. https://doi.org/10.1136/bmj.39489.470347.Advertizing
-
Urschel JD, Scott PG, Williams HTG (1988) Etiology of belatedly developing incisional hernias — the possible role of mechanical stress. Med Hypotheses 25(one):31–34. https://doi.org/10.1016/0306-9877(88)90043-vi
-
Muysoms FE, Antoniou SA, Coffin Thousand et al (2015) European Hernia Club guidelines on the closure of abdominal wall incisions. Hernia 19(1):1–24. https://doi.org/10.1007/s10029-014-1342-v
-
Gerten KA, Richter HE, Wheeler TL et al (2008) Intraabdominal force per unit area changes associated with lifting: implications for postoperative activity restrictions. Am J Obstet Gynecol 198(iii):306.e1–v. https://doi.org/10.1016/j.ajog.2007.09.004
-
Iqbal A, Haider M, Stadlhuber RJ et al (2008) A study of intragastric and intravesicular pressure changes during residual, cough, weight lifting, retching, and vomiting. Surg Endosc 22(12):2571–2575. https://doi.org/10.1007/s00464-008-0080-0
-
Weir LF, Nygaard IE, Wilken J et al (2006) Postoperative activity restrictions. Obstet Gynecol 107(2):305–309. https://doi.org/ten.1097/01.AOG.0000197069.57873.d6
-
Cobb WS, Burns JM, Kercher KW et al (2005) Normal intraabdominal pressure in healthy adults. J Surg Res 129(2):231–235. https://doi.org/10.1016/j.jss.2005.06.015
-
Lau FH, Pomahac B (2014) Wound healing in acutely injured fascia. Wound Repair Regen 22(Suppl 1):14–17. https://doi.org/10.1111/wrr.12165
-
Dubay DA, Wang X, Kirk South et al (2004) Fascial fibroblast kinetic action is increased during abdominal wall repair compared to dermal fibroblasts. Wound Repair Regen 12(5):539–545. https://doi.org/10.1111/j.1067-1927.2004.012506.x
-
Franz MG, Smith PD, Wachtel TL et al (2001) Fascial incisions heal faster than skin: a new model of abdominal wall repair. Surgery 129(2):203–208. https://doi.org/x.1067/msy.2001.110220
-
Höer J, Lawong 1000, Klinge U et al (2002) Einflussfaktoren der NarbenhernienentstehungRetrospektiveUntersuchung an 2.983 laparotomiertenPatientenübereinenZeitraum von 10 Jahren. Chirurg 73(v):474–480. https://doi.org/ten.1007/s00104-002-0425-5
-
Fink C, Baumann P, Wente MN et al (2014) Incisional hernia charge per unit 3 years afterwards midline laparotomy. Br J Surg 101(2):51–54. https://doi.org/x.1002/bjs.9364
-
Klinge U, Binnebösel M, Mertens PR (2006) Are collagens the culprits in the development of incisional and inguinal hernia illness? Hernia ten(vi):472–477. https://doi.org/10.1007/s10029-006-0145-8
-
Franz MG (2008) The biology of hernia formation. SurgClin Due north Am 88(1):one–fifteen. https://doi.org/10.1016/j.suc.2007.ten.007
-
Jairam AP, Timmermans L, Eker HH et al (2017) Prevention of incisional hernia with safety onlay and sublay mesh reinforcement versus primary suture merely in midline laparotomies (PRIMA): 2-year follow-up of a multicentre, double-blind, randomised controlled trial. The Lancet 390(10094):567–576. https://doi.org/x.1016/S0140-6736(17)31332-half-dozen
Funding
Open Access funding enabled and organized by Projekt Bargain.
Author information
Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors have zilch to declare.
Ideals approval
Counseling by the advisable ethics committee (Ethikkommission der Landesärztekammer Rheinland-Pfalz) revealed there was no ethics approval required.
Consent to participate
Participants were asked for their voluntary consent prior to taking part in the survey.
Additional information
Publisher'southward Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open up Access This article is licensed under a Creative Commons Attribution four.0 International License, which permits apply, sharing, accommodation, distribution and reproduction in any medium or format, as long as you give advisable credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were fabricated. The images or other third political party fabric in this article are included in the article's Artistic Eatables licence, unless indicated otherwise in a credit line to the fabric. If cloth is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, y'all will need to obtain permission directly from the copyright holder. To view a re-create of this licence, visit http://creativecommons.org/licenses/by/iv.0/.
Reprints and Permissions
Most this article
Cite this article
Schaaf, Due south., Willms, A., Schwab, R. et al. Recommendations on postoperative strain and physical labor later abdominal and hernia surgery: an expert survey of attendants of the 41st EHS Annual International Congress of the European Hernia Society. Hernia (2021). https://doi.org/x.1007/s10029-021-02377-west
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1007/s10029-021-02377-w
Keywords
- Abdominal surgery
- Hernia surgery
- Postoperative strain
- Incisional hernia
Source: https://link.springer.com/article/10.1007/s10029-021-02377-w
0 Response to "When Can You Lift Weights After Hernia Surgery"
Post a Comment